|
Overview In operational settings, most women
complaining of vaginal discharge will have no other associated
symptoms (pain, bleeding, fever, vulvar lesions, etc.) You can solve
95% of these vaginal discharge complaints by asking two questions:
- Does it itch?
- Does it have a bad odor?
If it itches, give the patient Monistat (or other antifungal
medication). If there is a bad odor, give Flagyl. If it itches and has
a bad odor, give both Monistat and Flagyl. You will solve most of the
vaginal discharge problems and will miss nothing important for very
long.
Those women whose symptoms persist despite this expedient treatment
will need a more thorough evaluation. For those, the diagnosis of
vaginal discharge is based on a History, Physical Exam, and a few
simple diagnostic tests.
History
Ask the patient about itching, odor, color of discharge, painful
intercourse, or spotting after intercourse.
- Yeast causes intense itching with a cheesy, dry discharge.
- Gardnerella causes a foul-smelling, thin white discharge.
- Trichomonas gives irritation and frothy white discharge.
- Foreign body (lost tampon) causes a foul-smelling black
discharge.
- Cervicitis causes a nondescript discharge with deep dyspareunia
- Chlamydia may cause a purulent vaginal discharge, post-coital
spotting, and deep dyspareunia.
- Gonorrhea may cause a purulent vaginal discharge and deep
dyspareunia.
- Cervical ectropion causes a mucous, asymptomatic discharge.
Vaginal Itching and Discharge
MS PowerPoint
22 Slides
2.5 MB ppt file
Free Download Now
|
|
 Physical Exam
Inspect carefully for the presence of lesions, foreign bodies and
odor. Palpate to determine cervical tenderness.
- Yeast has a thick white cottage-cheese discharge and red vulva.
- Gardnerella has a foul-smelling, thin discharge.
- Trichomonas has a profuse, bubbly, frothy white discharge.
- Foreign body is obvious and has a terrible odor.
- Cervicitis has a mucopurulent cervical discharge and the cervix
is tender to touch.
- Chlamydia causes a friable cervix but often has no other
findings.
- Gonorrhea causes a mucopurulent cervical discharge and the
cervix may be tender to touch.
- Cervical ectropion looks like a non-tender, fiery-red, friable
button of tissue surrounding the cervical os.
- Infected/Rejected IUD demonstrates a mucopurulent cervical
discharge in the presence of an IUD. The uterus is mildly tender.
- Chancroid appears as an ulcer with irregular margins, dirty-gray
necrotic base and tenderness.
Laboratory
Obtain cultures for chlamydia, gonorrhea, and Strept.
You may test the vaginal discharge in any of 4 different ways:
-
Test the pH. If >5.0, this suggests Gardnerella.
-
Mix one drop of KOH with some of the discharge on a
microscope slide. The release of a bad-smelling odor confirms
Gardnerella.
-
Examine the KOH preparation under the microscope
("Wet Mount"). Multiple strands of thread-like hyphae confirm the
presence of yeast.
-
Mix one drop of saline with some discharge ("Wet
Mount"). Under the microscope, large (bigger than WBCs), moving
micro-organisms with four flagella are trichomonads. Vaginal
epithelial cells studded with coccoid bacteria are "clue cells"
signifying Gardnerella.
Treatment
In addition to specific treatment of any organism
identified by culture or other test...
-
Any patient complaining of an itchy vaginal
discharge should probably be treated with an antifungal agent
(Monistat, Lotrimin, etc.) because of the high likelihood that yeast
is present, and
-
Any patient complaining of a bad-smelling vaginal
discharge should probably be treated with Flagyl (or other
reasonable substitute) because of the high likelihood that
Gardnerella is present.
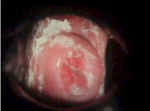
Ectropion, Erosion or Eversion
This harmless condition is frequently mistaken for
cervicitis.
Ectropion, erosion or eversion (all synonyms) occurs
when the normal squamo-columnar junction is extended outward from the
its; normal position at the opening of the cervix.
Grossly, the cervix has a red, friable ring of tissue
around the os. Careful inspection with magnification (6-10x) will
reveal that this red tissue is the normal tissue of the cervical
canal, which has grown out onto the surface of the cervix.
Cervical ectropion is very common, particularly in
younger women and those taking BCPs. It usually causes no symptoms and
need not be treated. If it is symptomatic, producing a more or less
constant, annoying, mucous discharge, cervical cauterization will
usually eliminate the problem.
When faced with a fiery red button of tissue
surrounding the cervical os, chlamydia culture (in high-risk
populations) and Pap smear should be performed. If these are negative
and the patient has no symptoms, this cervical ectropion should be
ignored.
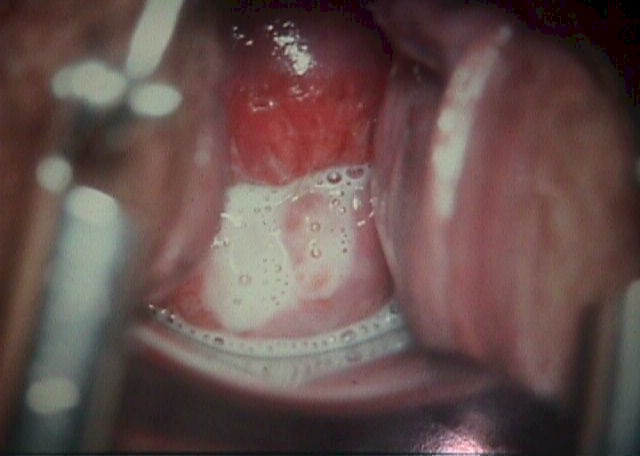
Cervicitis
Inflammation or irritation of the cervix is rarely the
cause of significant morbidity. It is mainly a nuisance to the patient
and a possible symptom of underlying disease (gonorrhea, chlamydia).
Some patients with cervicitis note a purulent vaginal
discharge, deep dyspareunia, and spotting after intercourse, while
others may be symptom-free. The cervix is red, slightly tender, bleeds
easily, and a mucopurulent cervical discharge from the os is usually
seen.
A Pap smear rules out malignancy. Chlamydia culture
and gonorrhea culture (for gram negative diplococci) are routinely
performed.
No treatment is necessary if the patient is
asymptomatic, the Pap smear is normal, and cultures are negative.
Antibiotics specific to the organism are temporarily effective and may
be curative. Cervical cautery may be needed to achieve permanent cure.
Continue
to the PowerPoint Lecture...
From:
Operational Obstetrics & Gynecology
2nd Edition
NAVMEDPUB 6300-2C
Bureau of Medicine and Surgery
Department of the Navy |


