|
Uncertainty of Diagnosis
When treating a female patient with abdominal pain, I
sometimes don't have a clue as to what the problem is. I say this as a
board-certified OB-GYN, with more than 20 years in clinical practice, practicing
in a 600-bed teaching hospital, with ultrasound, MRI scans, and full lab
support. Sometimes all I can say is: "This patient is sick with something."
Sometimes these patients get well before I can figure out
the diagnosis. Sometimes these patients get worse and I end up performing
surgery and find PID, or endometriosis, or an ovarian cyst or almost any other
gynecologic, surgical or medical problem. Sometimes I do laparoscopy and find
nothing abnormal, but the pain goes away.
The First Point is: In clinical gynecology, the
diagnosis is often unclear. Just because you're unsure of the diagnosis
doesn't mean you can't take good care of the patient. Often you must treat the
patient before knowing the diagnosis.
The Second Point is: More important than knowing
the correct diagnosis is doing the right thing for the patient.
|
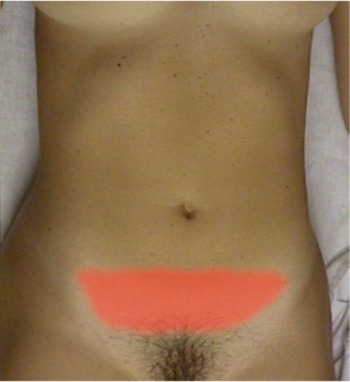
Pain and Bedrest
If the patient has pelvic/abdominal pain or
tenderness, placing her on bedrest for a few days will usually help and is
never the wrong thing to do. For many of your patients, the pain will simply
resolve (although you won't know why).
Pain and Fever
If the patient has a fever (in addition to her pain),
I would recommend you give her antibiotics to cover PID. With mild pain and
fever, oral antibiotics should work well, so long as they are effective
against chlamydia (Doxycycline, tetracycline, erythromycin, Azithromycin ,
etc.).
If the fever is high or the pain is moderate to severe, I
would recommend IV antibiotics (such as clindamycin/gentamicin or cefoxitin or
cefotetan or Flagyl/gentamicin) to cover the possibility of pelvic abscess.
Chronic Pain
If there is no fever, but your patient complains of
chronic pelvic pain, a course of oral Doxycycline is wise. Some of these women
will be suffering from chlamydia and you may cure them through the use of an
antibiotic effective against chlamydia. Others will not improve and will need
further evaluation by experienced providers in well-equipped settings.
Pregnancy Test
Any patient complaining of pelvic pain should have a
pregnancy test. I am surprised at how often it is positive despite the patient
saying "that's impossible."
BCPs and Pain
Most patients complaining of intermittent,
chronic pelvic pain will benefit from oral contraceptive pills. BCPs reduce or
eliminate most dysmenorrhea and have a favorable influence on other gynecologic
problems such as endometriosis, ovarian cysts, and adenomyosis, a benign
condition in which the uterine lining grows into the underlying muscle wall,
causing pain and heavy periods.
When using BCPs to treat chronic pelvic
pain, multiphasic BCPs such as Ortho Novum 7/7/7, Triphasil or Tri-Norinyl
have not been as effective as the stronger, monophasic BCPs such as LoOvral,
Ortho Novum 1+35 or Demulen 1/35 (in my experience). I believe the reason is
that the multiphasic pills, by virtue of their lower dose and changing
dosage, do not suppress ovulation as consistently as the higher-dose pills.
If the BCPs do not help or if the patient
continues to have pain during her menstrual flow, change the BCP schedule so
the patient takes a monophasic (LoOvral, 1+35, etc.) BCP every day. She
will:
-
not stop at the end of a pack.
-
not wait one week before restarting.
-
not have a menstrual flow.
If she doesn't have a menstrual flow, she
can't get dysmenorrhea. Taken continuously, BCPs are effective and safe. The
only important drawback is that she will not have a monthly menstrual flow
to reassure her that she is not pregnant.
Because the birth control pills are so
very effective in treating dysmenorrhea, the emergence of cyclic pelvic pain
while taking BCPs is a worrisome symptom. Endometriosis can cause these
symptoms. Happily, birth control pills, particularly if taken continuously,
are a very effective treatment for endometriosis. Upon return to a garrison
setting, women with pain while taking should be evaluated by an experienced
gynecologic clinician.
After a number of months, women on
continuous BCPs will usually experience spotting or breakthrough bleeding.
It is not dangerous. If this becomes a nuisance, stop the BCPs for one week
(she'll have a withdrawal bleed), and then restart the BCPs continuously.
Continue
to the PowerPoint Lecture...
From:
Operational Obstetrics & Gynecology
2nd Edition
NAVMEDPUB 6300-2C
Bureau of Medicine and Surgery
Department of the Navy
|