Operational Obstetrics & Gynecology
Human Papilloma Virus (HPV)
| Clinical Warts | Persistence of Virus | Relation to Cervical Cancer |
| Subclinical Warts | Transmission of Virus | Evaluation |
| Treatment | Relation to Cervical Dysplasia |
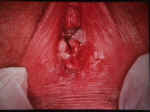 Condyloma acuminata, (venereal warts) are caused by a virus known as "Human
Papilloma Virus" (HPV).
Condyloma acuminata, (venereal warts) are caused by a virus known as "Human
Papilloma Virus" (HPV).
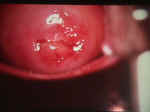
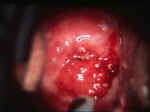
There are two categories of warts, clinical and subclinical. Clinical warts appear as tiny, cauliflower-like, raised lesions around the opening of the vagina or inside the vagina. These lesions appear flesh-colored or white, are not tender and have a firm to hard consistency. If they are on the outside of the vagina or vulva, they are generally symptomatic, causing itching, burning, and an uncomfortable sensation during intercourse. If they are inside the vagina, they generally cause no symptoms.
|
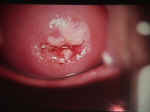
Apparently normal cervix After application of acetic acid |
The second category, subclinical warts, are invisible to the naked eye, are flat and colorless. They usually do not cause symptoms, although they may cause similar symptoms to the raised warts. These subclinical warts can be visualized if the skin is first soaked for 2-3 minutes with vinegar (3-4% acetic acid) and then viewed under magnification (4-10X) using a green or blue (red-free) light source.
Venereal warts are not dangerous and have virtually no malignant potential. Clinical warts may be a nuisance and so are usually treated. Subclinical warts are usually not treated since they are not a nuisance (most people with subclinical warts are unaware of their presence).
Treatment consists of removal of the wart. This can be accomplished in any number of ways, some more painful than others:
- Apply a small amount of bichloracetic acid (80-90%) directly to the wart, taking care to avoid spreading the acid onto the normal surrounding skin. For larger lesions, use a cotton-tipped applicator dipped in the acid. For smaller lesions, use the "stick" end of the cotton-tipped applicator. Apply enough acid (very tiny amounts) to cause the lesion to turn white, but not so much that it runs down onto the normal surrounding skin. No anesthetic is necessary. The patient may feel nothing, some slight tingling, or a minor stinging. After a minute or two, rinse the skin with warm water to dilute any remaining acid and prevent it from coming into contact with the surrounding skin.
Try to use less acid than you think will be effective since the patient would rather return for a second, third or fourth treatment than recover from a serious acid burn of the vulva. Don't use acid inside the vagina or on the cervix.
Cryosurgery can effectively remove warts. Freezing the wart with any convenient tool (liquid nitrogen, cryosurgical probe, etc.) can be done without anesthetic and results in sloughing of the wart in a week or two. Be careful not to freeze normal skin. Two freeze-thaw cycles usually work better than a single freeze-thaw cycle.
Cryosurgery should not be done inside the vagina or on the cervix unless you have been specially trained to do this as damage to other structures can occur.
Watch a video on cryosurgery of warts
- Podophyllum resin can be applied directly to the wart, followed by washing off the residual podophyllin in 3-6 hours. This effective approach runs the risk of podophyllin toxicity. This is a minor issue if the wart is very small and you use tiny quantities of podophyllin. If you use large amounts, or apply it inside the vagina, toxicity is a real issue.
Don't apply large amounts of podophyllin and don't apply any inside the vagina or on the cervix.
- Under anesthetic, warts can be surgically removed, burned, or electrocuted, but such methods are usually unnecessary for the typical small wart(s).
- If untreated, many warts will gradually resolve and disappear spontaneously, but this may require many months or years.
Remember that in treating the warts, you are actually destroying the patient's skin which has responded in a strange and annoying way to the presence of the HPV. You are not getting rid of the HPV itself.
HPV is a sexually-transmitted virus which usually causes no symptoms but occasionally causes warts. The virus spreads throughout the skin of the vulva and vagina (as well as the inner thighs and lower abdomen), where it disappears into the skin cells and usually remains dormant forever. Like many other viruses, if the patient's immune system allows the virus to grow, it can reappear and cause warts. This virus is extremely common, infecting as many as 1/3 of the adult, sexually-active population. There is no known way to eliminate the virus from all skin cells.
Patients with HPV are contagious to others, but there is no effective way to prevent its spread. Some physicians recommend condoms, but because the virus is found in areas of the skin beyond the condom, this is not likely to be effective. Some physicians recommend aggressive treatment of all warts, in the belief that active warts are more contagious than inactive virus within the skin. This theory has not, so far, been proven to be true.
While warts are not considered dangerous, HPV infection is associated with another skin change known as "dysplasia." Dysplasia means that the skin (mainly of the cervix) begins growing faster than it should. There are different degrees of dysplasia: mild, moderate and severe. None of these is malignant, but it is true that the next step beyond severe dysplasia is cancer of the cervix.
About 1/3 of all adult, sexually-active women have been infected with HPV, but probably less than 10% will ever develop dysplasia. Most (90%) of those with dysplasia will have mild dysplasia which will either regress back to normal or at least will never progress to a more advanced stage.
|
Invasive Cancer of the Cervix |
Most women (About 90%) with mild dysplasia of the cervix will never develop a more advanced problem, and often the abnormality regresses back to normal.
Most women with moderate to severe dysplasia of the cervix, if left untreated, will ultimately develop cancer of the cervix. If treated, most of these abnormalities will revert to normal, making this form of cervical cancer largely preventable.
Cervical dysplasia is usually a slowly-changing clinical problem. There is indirect evidence to suggest that on average, it takes about 10 years to advance from normal, through the various stages of dysplasia, and into cancer of the cervix. Of course, any individual may not follow these rules. In providing medical care to women with cervical dysplasia, good follow-up is important, but urgent medical evacuation is usually not indicated for less threatening categories of dysplasia.
In any patient with venereal warts (condyloma), you should look for possible dysplasia of the cervix. This is best done with colposcopy, but a simple Pap smear can be very effective. Because HPV causes warts and is also associated with dysplasia, more frequent Pap smears (every 6 months) is a wise precaution, at least initially.
If dysplasia is found, gynecologic consultation will be necessary, although this may be safely postponed for weeks or months if operational requirements make consultation difficult.
Home À Introduction À Medical Support of Women in Field Environments À The Prisoner of War Experience À Routine Care À Pap Smears À Human Papilloma Virus À Contraception À Birth Control Pills À Vulvar Disease À Vaginal Discharge À Abnormal Bleeding À Menstrual Problems À Abdominal Pain À Urination Problems À Menopause À Breast Problems À Sexual Assault À Normal Pregnancy À Abnormal Pregnancy À Normal Labor and Delivery À Problems During Labor and Delivery À Care of the Newborn
|
Bureau of Medicine
and Surgery |
Operational
Obstetrics & Gynecology - 2nd Edition |
This web version of Operational Obstetrics & Gynecology is provided by The Brookside Associates Medical Education Division. It contains original contents from the official US Navy NAVMEDPUB 6300-2C, but has been reformatted for web access and includes advertising and links that were not present in the original version. This web version has not been approved by the Department of the Navy or the Department of Defense. The presence of any advertising on these pages does not constitute an endorsement of that product or service by either the Department of Defense or the Brookside Associates. The Brookside Associates is a private organization, not affiliated with the United States Department of Defense. All material in this version is unclassified.
This formatting ® 2006
Medical Education Division,
Brookside Associates, Ltd.
All rights reserved