|
|
Operational Obstetrics & Gynecology
Labor and Delivery
Watch a Video Showing a Normal Delivery or Cesarean Section
Electronic fetal monitors continuously record the instantaneous fetal heart rate on the upper channel and uterine contractions on the lower channel. They do this by attaching, either externally (and non-invasively) or internally, to detect the fetal heart and each uterine contraction.
A normal contraction pattern in active labor shows contractions occurring about every 2-3 minutes and lasting about 60 seconds.
The normal fetal heart rate baseline is 120-160 BPM and has both short and long-term "variability." Short term variability means that from one moment to the next, the fetal heart speeds up slightly and then slows down slightly, usually with a range of 3-5 BPM from the baseline.
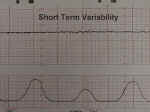 Short Term Variability |
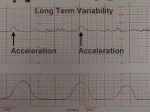 Long Term Variability |
Reduced variability occurs normally during fetal sleep and usually returns after 20 to 40 minutes. It also may be present with fetal anomalies or injury. Persistent or progressively reduced variability is not, by itself, a sign of fetal jeopardy. But in combination with other abnormalities (see below), it may indicate fetal intolerance of labor.
Long-term variability represents broad-based swings in fetal heart rate, or "waviness," occurring up to several times a minute. One form of long-term variability of particular significance is a fetal heart "acceleration." These usually occur in response to fetal movement, and are 15 BPM above the baseline or more, lasting 10-20 seconds or longer. They can often be provoked by stimulating the fetal scalp during a pelvic examination, or by acoustically stimulating the fetus with a loud, obnoxious noise. The presence of fetal accelerations is reassuring that the fetus is healthy and tolerating the intrauterine environment well.
During labor, no significance is attached to the absence of fetal accelerations.
Tachycardia is the sustained elevation of fetal heart rate baseline above a 160 BPM. Most tachycardias are not indicative of fetal jeopardy. Causes include:
|
|
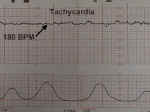 Tachycardia |
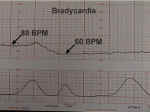 Bradycardia |
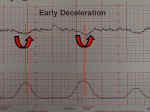 Early Deceleration |
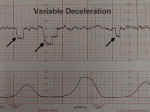 Variable Deceleration |
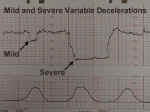 Mild and Severe Variable Decelerations |
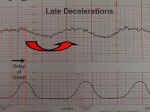 Late Deceleration |
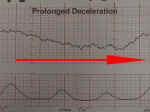 Prolonged Deceleration |
Bradycardia is the sustained depression of fetal heart rate baseline below 120 BPM. Most of these are caused by increased vagal tone, although congenital cardiac abnormalities can also be responsible.
Mild bradycardia (to 80 or 90 BPM) with retention of beat-to-beat variability is common during the second stage of labor and not of great concern so long as delivery occurs relatively soon. Moderate to severe bradycardia (below 80 BPM) with loss of beat-to-beat variability, particularly in association with late decelerations, is more troubling and may indicate fetal distress, requiring prompt resolution.
Early decelerations are periodic slowing of the fetal heartbeat, synchronized exactly with the contractions. These dips are rarely more than 20 or 30 BPM below the baseline.
These innocent changes are thought to be due, in many cases, to fetal head compression within the birth canal.
Variable decelerations are variable in onset, duration and depth. They may occur with contractions or between contractions.
Typically, they have an abrupt onset and rapid recovery (in contrast to other types of decelerations which gradually slow and gradually recover.
Variable decelerations are thought to represent a vagal response to some degree of umbilical cord compression. They are not caused by hypoxia, although if severe enough, frequent enough and persistent enough, can ultimately lead to some degree of fetal acidosis.
Mild or moderate variable decelerations are common and not considered threatening.
Mild variable decelerations do not dip below 70 BPM and last less than 30 seconds.
Severe variable decelerations dip below 60 BPM for at least 60 seconds ("60 x 60"). If persistent and not correctable by simple means, they can be threatening to fetal well-being.
Late decelerations are repetitive, gradual slowings of the fetal heartbeat toward the end of the contraction cycle. They are felt to represent some degree of utero-placental insufficiency.
If persistent and not correctable, they represent a threat to fetal well-being.
Prolonged decelerations last more than 60 seconds and occur in isolation. Causes include maternal supine hypotension, epidural anesthesia, paracervical block, tetanic contractions, and umbilical cord prolapse.
Some of these are largely self-correcting, such as the deceleration following paracervical block, while others (maternal supine hypotension) respond to simple measures such as repositioning.
Other causes (such as umbilical cord prolapse) require prompt intervention to avoid or reduce the risk of fetal injury.
Home À Introduction À Medical Support of Women in Field Environments À The Prisoner of War Experience À Routine Care À Pap Smears À Human Papilloma Virus À Contraception À Birth Control Pills À Vulvar Disease À Vaginal Discharge À Abnormal Bleeding À Menstrual Problems À Abdominal Pain À Urination Problems À Menopause À Breast Problems À Sexual Assault À Normal Pregnancy À Abnormal Pregnancy À Normal Labor and Delivery À Problems During Labor and Delivery À Care of the Newborn
|
Bureau of Medicine
and Surgery |
Operational
Obstetrics & Gynecology - 2nd Edition |
 This
web version of Operational Obstetrics & Gynecology is provided by
The Brookside Associates
Medical Education Division. It contains original contents from the
official US Navy NAVMEDPUB 6300-2C, but has been reformatted for web access and
includes advertising and links that were not present in the original version.
This web version has not been approved by the Department of the Navy or the
Department of Defense. The presence of any advertising on these pages does not
constitute an endorsement of that product or service by either the Department of
Defense or the Brookside Associates. The Brookside Associates is a private
organization, not affiliated with the United States Department of Defense. All
material in this version is unclassified.
This
web version of Operational Obstetrics & Gynecology is provided by
The Brookside Associates
Medical Education Division. It contains original contents from the
official US Navy NAVMEDPUB 6300-2C, but has been reformatted for web access and
includes advertising and links that were not present in the original version.
This web version has not been approved by the Department of the Navy or the
Department of Defense. The presence of any advertising on these pages does not
constitute an endorsement of that product or service by either the Department of
Defense or the Brookside Associates. The Brookside Associates is a private
organization, not affiliated with the United States Department of Defense. All
material in this version is unclassified.
This formatting ® 2006
Medical Education Division,
Brookside Associates, Ltd.
All rights reserved